Advice is evolving along with the coronavirus. Here's the latest from staff and wire reports.
What's the latest?
July 4th was a COVID-19 spreader in Minnesota, though illnesses far below pandemic peaks.
COVID is on the rise in Minnesota. Here's how to stay safe amid a spike.
Vaccines significantly reduce the risk of long COVID, study finds.
Gastrointestinal issues are a common but often unrecognized sign of infection.
COVID on the rise everywhere else — is Minnesota next?
New COVID shots are recommended for Americans 6 months and older this fall.
COVID will still be here this summer. Will anyone care?
Is it COVID, spring allergies or a cold?
For most of this year, the JN.1 variant of the coronavirus accounted for an overwhelming majority of COVID-19 cases. But now an offshoot variant called KP.2 is taking off.
Thousands believe COVID vaccines harmed them. Is anyone listening?
The Minnesota Supreme Court ruled as constitutional the law under which Gov. Tim Walz declared a peacetime emergency during the COVID-19 pandemic.
Patients with COVID-19 had lower viral loads if treated with metformin, according to new University of Minnesota research that argues for broader use of the cheap anti-diabetes drug and against the controversial use of ivermectin.
Pharmacies received emergency authority during the COVID-19 pandemic to vaccinate most Minnesotans, and now they want funding and permission to make that gig permanent.
A M Health Fairview clinic is confronting an exhausting disorder that has afflicted more children since the pandemic and caused alarming spikes in heart rate, blood pressure and breathing.
An analysis of mortality statistics suggests the death count in the United States from COVID-19 is higher than the 1.1 million officially linked to the disease, according to University of Minnesota research.
Omicron, now two years old, has proved to be not only staggeringly infectious, but an evolutionary marvel. Read more here.
What Minnesotans should know about the new COVID-19 vaccine, targeted to the omicron descendant XBB.1.5.
Mayo Clinic is reporting an additional benefit of vaccination beyond protection from COVID-19 infection — a lower likelihood of severe symptoms if people end up with long COVID.
Some people who experience cognitive issues after long COVID continue to struggle with brain function for at least two years, a study shows. Research shows a majority of people experiencing long COVID symptoms have reported brain fog — a collection of symptoms, including impaired attention, concentration, memory and processing speed. Read more here.
A study published in the scientific journal Nature suggests people with a specific version of a gene were far more likely to experience an asymptomatic infection than those without. The relevant set of genes is known as the human leukocyte antigen, or HLA. Read more here.
What are symptoms?
Symptoms include sore throat, runny nose, coughing, head and body aches, fever, congestion, fatigue and, in severe cases, shortness of breath. Fewer people lose their sense of taste and smell now than did at the start of the pandemic.
Dr. Peter Chin-Hong, an infectious disease specialist at the University of California, San Francisco, said that patients were often surprised that diarrhea, nausea and vomiting could be COVID symptoms as well and that they sometimes confused those issues as signs that they had norovirus.
Where can I get tested for COVID-19?
The Minnesota Department of Health's free COVID-19 at-home test ordering program has ended. People who do not have health insurance can find no-cost tests using the CDC's COVID-19 Testing Locator. You may find home rapid tests at pharmacies including Walgreens and CVS, grocery stores, health care providers and online.
Where can I see Minnesota COVID-19 updates?
See Minnesota's weekly pandemic update with new numbers Thursdays at 11 a.m.
How do I get antiviral treatments?
Oral antivirals are no longer being distributed by the federal government but are available in pharmacies for free or at low cost for the majority of patients until the end of 2024, according to the Minnesota Department of Health. There is also a new monoclonal antibody treatment called Pemgarda that has been authorized for the prevention of serious illness from COVID-19 in people who have a suppressed immune system. For more information, go to MDH: COVID-19 Medications.
Where can I get a vaccine?
Check the state of Minnesota's vaccine page or vaccines.gov. The white COVID-19 vaccination cards have been phased out, now that vaccines are not being distributed by the federal government.
How can I make a COVID-19 vaccine appointment for kids in Minnesota?
Minnesota has a webpage (mn.gov/vaxforkids) to help parents and guardians find a vaccine and answer questions. U.S. regulators cleared doses of the updated COVID-19 vaccines for children younger than age 5. Read CDC vaccine advice here.
What should I do if I've been exposed?
To be confident you do not have COVID-19, FDA recommends two negative antigen tests for individuals with symptoms or three antigen tests for those without symptoms, performed 48 hours apart. Read more here.
The CDC updated its guidance March 1 to adopt a unified approach to addressing common respiratory viral illnesses, such as COVID-19, flu and RSV.
What should I do if I test positive for COVID-19?
If you feel sick, stay home and away from others until 24 hours after you are fever-free (without fever-reducing medications) and your symptoms are getting better, according to Minnesota Department of Health guidelines. (The Mayo Clinic has guidelines for home care here.) Then layer on added prevention strategies (such as masks, distancing and tests) for the next five days. Talk to your doctor right away about medications that can help you recover faster, especially if you are in a high-risk group.
How does getting vaccinated affect the menstrual cycle?
A study of nearly 20,000 people around the world shows that getting vaccinated against COVID can change the timing of the menstrual cycle. Vaccinated people experienced, on average, about a one-day delay in getting their periods, compared with those who hadn't been vaccinated.
What is the Novavax vaccine?
Novavax shots — used in Australia, Canada, parts of Europe and dozens of other countries — are a protein vaccine that's made with a more conventional technology than the other U.S. options. Protein vaccines have been used for years to prevent other diseases including hepatitis B and shingles.
How do variants work?
At first, SARS-CoV-2 followed the slow and steady course that scientists had expected based on other coronaviruses. Its evolutionary tree gradually split into branches, each gaining a few mutations. Evolutionary biologists kept track of them with codes.
But then one lineage, initially known as B.1.1.7, defied expectations. When British scientists discovered it, in December 2020, they were surprised to find it bore a unique sequence of 23 mutations. Those mutations allowed it to spread much faster.
Within a few months, several other worrying variants came to light around the world — each with its own combination of mutations, each with the potential to spread quickly and cause a surge of deaths. To make it easier to communicate about them, the WHO came up with its Greek system. B.1.1.7 became alpha.
Alpha came to dominate the world, whereas beta took over only in South Africa and a few other countries before petering out. Beta did not descend from alpha. Instead, it arose with its own set of new mutations from a different branch of the SARS-CoV-2 tree. The same held true for all the Greek-named variants, up to omicron.
It's likely that most of these variants got their mutations by going into hiding. Instead of jumping from one host to another, they created chronic infections in people with weakened immune systems. These victims harbored the virus for months, allowing it to accumulate mutations. When it eventually emerged from its host, the virus had a startling range of new abilities — finding new ways to invade cells, weaken the immune system and evade antibodies.
What is the omicron variant?
First identified in Botswana and South Africa in November 2021, the omicron variant surged around the world. Scientists first recognized omicron thanks to its distinctive combination of more than 50 mutations. Some of them were carried by earlier variants such as alpha and beta. Read more here.
All the most significant COVID-19 variations today are descending from omicron. After the original omicron virus evolved in the fall of 2021, its descendants split into at least five branches, known as BA.1 through BA.5. As it spread and caused an unprecedented spike in cases, it drove most other variants to extinction. Over the next few months, the subvariants took turns rising to dominance.
What is KP.2?
KP.2 belongs to a subset of COVID variants scientists have nicknamed "FLiRT," drawn from the letters in the names of their mutations. They are descendants of JN.1, and KP.2 is "very, very close" to JN.1, said Dr. David Ho, a virus expert at Columbia University.
Experts said that even if you had JN.1, you may still get reinfected with KP.2 — particularly if it's been several months or longer since your last bout of COVID. KP.2 could infect even people who got the most updated vaccine, Ho said, since that shot targets XBB.1.5, a variant that is notably different from JN.1 and its descendants. Still, the shot does provide some protection, especially against severe disease, doctors said, as do previous infections.
What is JN.1?
JN.1 is the fastest-growing variant to emerge in past two years. The World Health Organization designated it a variant of interest due to its rapid growth and potential to add to the respiratory virus burden in the Northern Hemisphere. The latest booster formulation should provide good protection against it, according to the organization.
The strain emerged in August from the ultra-mutated BA.2.86, or Pirola variant. While Pirola wasn't especially remarkable, a hallmark mutation that produced JN.1 has resulted in greater transmissibility and immune evasiveness, University of Tokyo scientists reported.
What is BA.2.86?
BA.2.86 stood out in the omicron family tree because of how much it morphed, with more than 30 mutations on its spike protein.
What is "Eris"?
The WHO in summer 2023 designated the omicron subvariant EG.5, which includes a similar EG.5.1 strain, as one of its "variants under monitoring." Twitter users and some media outlets nicknamed the subvariant "Eris." The virologist and researcher Stuart Turville, an associate professor at Sydney's University of New South Wales, called the EG.5 variant "a little bit more slippery" and "competitive" than its counterparts. Read more here.
What is Arcturus?
XBB.1.16, also known as Arcturus, is a subvariant of the omicron variant of COVID-19. It appears to be correlated with increased cases of conjunctivitis, the inflammation of the outer membrane of the eye better known as pink eye. Read more here.
What is the "kraken variant"?
XBB.1.5 is a descendant of the omicron XBB subvariant — which is itself a cross between two earlier strains: BA.2.75 and BA.2.10.1. Read more here.
What is "long COVID" and how many people get it?
Long COVID is the term used to describe an array of symptoms that can last for months or longer after the initial coronavirus infection. A study zeroed in on a dozen symptoms that may help define long COVID: fatigue; brain fog; dizziness; gastrointestinal symptoms; heart palpitations; sexual problems; loss of smell or taste; thirst; chronic cough; chest pain; worsening symptoms after activity and abnormal movements.
The federal definition of long COVID is symptoms that linger for four or more weeks. Cases vary in their duration, intensity and symptoms, but they often involve fatigue, headaches, dizziness and cognitive problems (or brain fog) — especially after exertion or exercise.
About 10% of people appear to suffer long COVID after an omicron infection, a lower estimate than earlier in the pandemic, according to a study published in the Journal of the American Medical Association.
Some people who experience cognitive issues after long COVID continue to struggle with brain function for at least two years, a study shows. In the United States, millions of people have reported symptoms of long COVID. Research shows a majority of people experiencing long COVID symptoms have reported brain fog — a collection of symptoms, including impaired attention, concentration, memory and processing speed. Read more here.
The Defense Department will buy an Edina firm's drug for radiation exposure that could also treat long COVID.
There is evidence that vaccination may reduce the chances of developing long COVID.
How often do COVID vaccines cause heart problems in kids?
While the COVID-19 vaccines made by Pfizer-BioNTech and Moderna do seem to be associated with an increased risk of myocarditis, the latest data indicate that the absolute risk remains very small and that most cases are mild and resolve quickly. Read more here.
Do masks work?
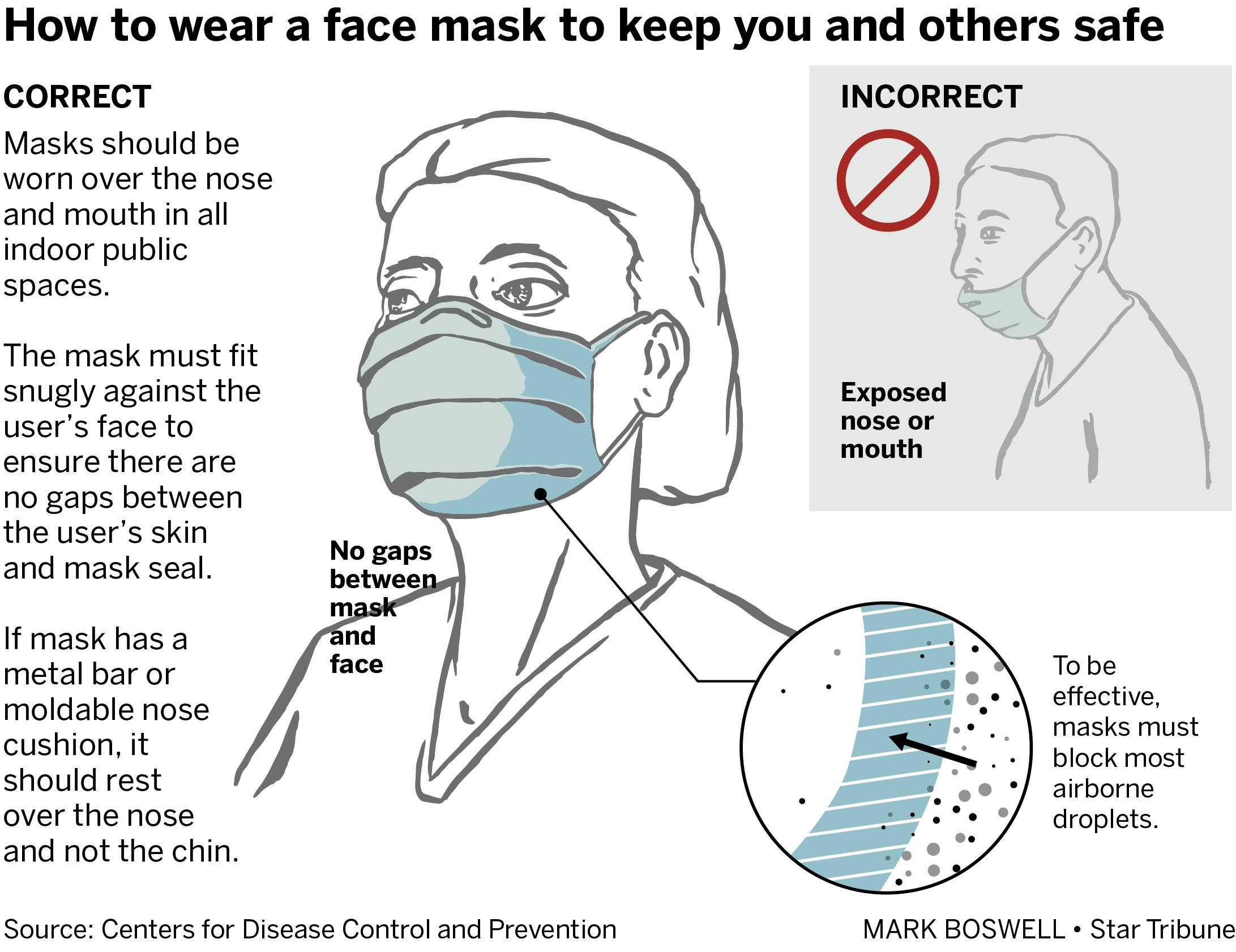
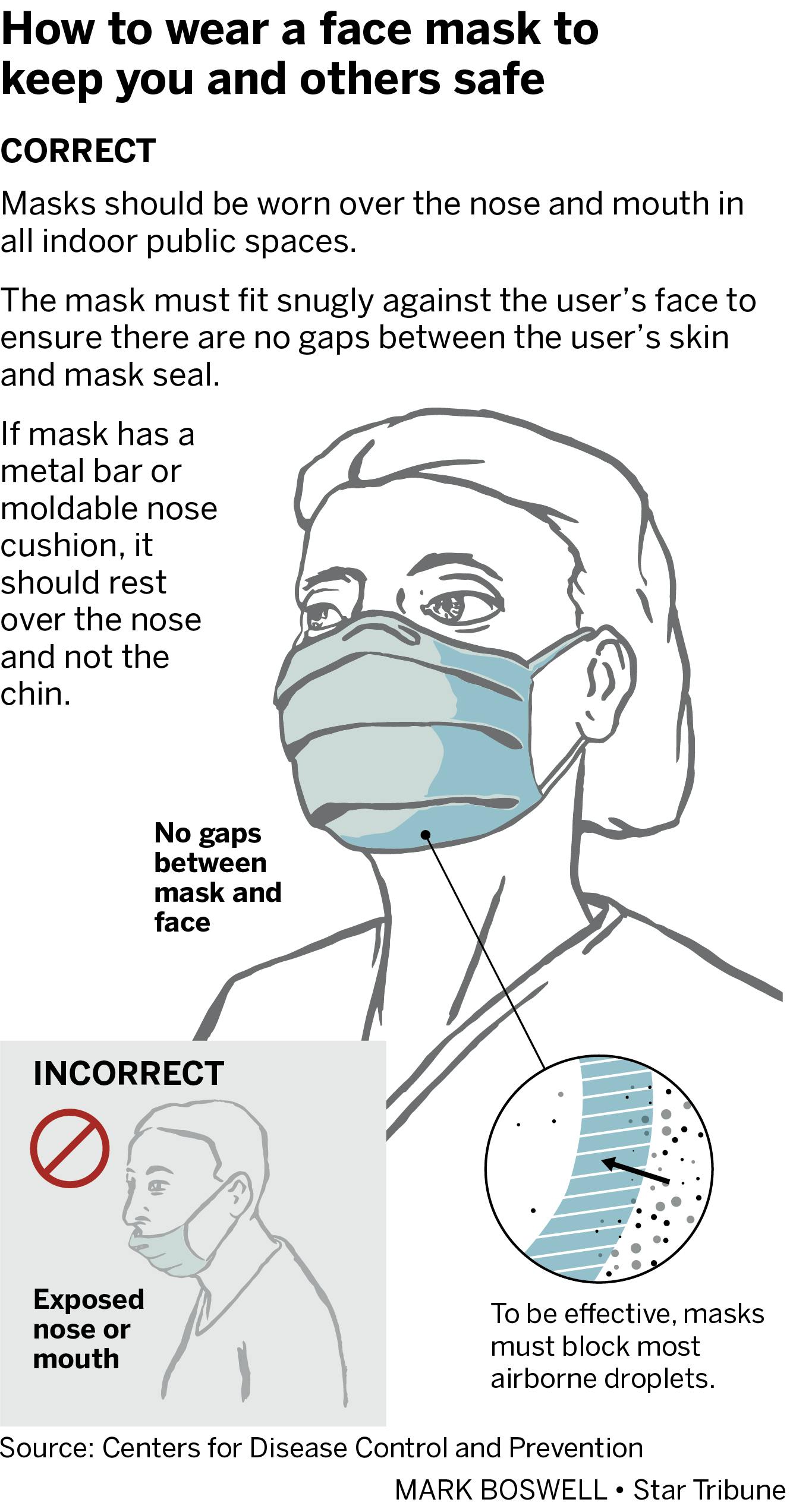
Ordinary surgical and paper masks work when worn properly, said Chris Hogan, a University of Minnesota researcher who has studied mask effectiveness and is editor of the Journal of Aerosol Science.
Generally, the CDC says masks should "fit snugly over your mouth, nose and chin."
If you decide to keep wearing your multi-layer homemade or cloth mask, experts advise washing them every day. But proceed with caution. Read more here.
What about N95s?
Masks are best at keeping your exhaled particles away from others. Respirators, like the N95, also keep others' particles away from you. Any bona fide N95 has been certified to filter at least 95% of particles.
Many doctors and public health experts are now advocating for their use among the general public. Early in the pandemic, people were discouraged the masks over fear there wouldn't be enough for health care workers. That's no longer the case. Read more about N95 and KN95 respirators here.
How does pregnancy affect immunity?
Pregnant women who are vaccinated are nearly twice as likely to get COVID-19 as those who are not pregnant, according to a study, and have the greatest risk among a dozen medical states, including being an organ transplant recipient and having cancer.
Dr. David R. Little, a researcher at Wisconsin-based Epic, said the findings buttress CDC recommendations that additional precautions against the virus should be taken during pregnancy, such as wearing masks and maintaining safe distances. Read more here.
Should pregnant women get the vaccine?
The CDC urged all pregnant women to get the COVID-19 vaccine. Expectant women run a higher risk of severe illness and pregnancy complications from the coronavirus.
A research study based on data from Bloomington-based HealthPartners and medical centers across the country finds that pregnant women who received COVID-19 vaccines did not experience an increased risk of miscarriage.
If you're thinking of getting pregnant, there's no evidence that any vaccines, including COVID-19 vaccines, influence your chances of getting pregnant despite a myth suggesting otherwise.
Do pregnant women who get vaccinated pass the protection to their babies?
COVID-19 vaccines during pregnancy can protect babies after they're born and lead to fewer hospitalized infants, a U.S. government study suggested.
Are the vaccines safe?
A review of 6.2 million vaccine recipients in Minnesota and seven other U.S. regions found no significantly elevated rates of conditions such as stroke or heart attack immediately following COVID-19 vaccination. Bloomington-based HealthPartners participated in the study, which looked for elevated rates of 23 potential side effects in the first three weeks after people received Pfizer or Moderna COVID-19 vaccines.
What's going on with Johnson & Johnson shots?
U.S. regulators strictly limited who can receive Johnson & Johnson's COVID-19 vaccine due to the ongoing risk of rare but serious blood clots. The FDA said the shot should be given only to adults who cannot receive a different vaccine or specifically request J&J's vaccine.
Can I get a vaccine incentive?
Those programs have ended.
Who qualifies for an extra shot?
Federal officials approved an extra dose for those undergoing cancer treatment, who've received organ transplants or had other conditions that depress the body's immune system. These doses are not considered to be boosters.
Can kids get long COVID?
Yes, but studies indicate they're less likely than adults to be affected by symptoms.
Kids can develop other rare problems after a coronavirus infection, including heart inflammation or a condition known as multisystem inflammatory syndrome. Because of the potential for long-term consequences, the American Academy of Pediatrics recommends follow-up doctor visits after children recover from an initial coronavirus infection.
What is the Docket app?
Minnesota introduced the Docket app for viewing personal immunization records in response to rising demand — largely because of COVID-19 vaccination requirements by employers and organizations.





